113173
论文已发表
注册即可获取德孚的最新动态
IF 收录期刊
- 3.4 Breast Cancer (Dove Med Press)
- 3.2 Clin Epidemiol
- 2.6 Cancer Manag Res
- 2.9 Infect Drug Resist
- 3.7 Clin Interv Aging
- 5.1 Drug Des Dev Ther
- 3.1 Int J Chronic Obstr
- 6.6 Int J Nanomed
- 2.6 Int J Women's Health
- 2.9 Neuropsych Dis Treat
- 2.8 OncoTargets Ther
- 2.0 Patient Prefer Adher
- 2.2 Ther Clin Risk Manag
- 2.5 J Pain Res
- 3.0 Diabet Metab Synd Ob
- 3.2 Psychol Res Behav Ma
- 3.4 Nat Sci Sleep
- 1.8 Pharmgenomics Pers Med
- 2.0 Risk Manag Healthc Policy
- 4.1 J Inflamm Res
- 2.0 Int J Gen Med
- 3.4 J Hepatocell Carcinoma
- 3.0 J Asthma Allergy
- 2.2 Clin Cosmet Investig Dermatol
- 2.4 J Multidiscip Healthc

The epidemiology of polypharmacy in older adults: register-based prospective cohort study
Authors Morin L, Johnell K, Laroche ML, Fastbom J, Wastesson JW
Received 7 October 2017
Accepted for publication 28 December 2017
Published 12 March 2018 Volume 2018:10 Pages 289—298
DOI https://doi.org/10.2147/CLEP.S153458
Checked for plagiarism Yes
Review by Single-blind
Peer reviewers approved by Dr Amy Norman
Peer reviewer comments 4
Editor who approved publication: Professor Vera Ehrenstein
Objective: Polypharmacy is the concomitant use of several drugs by a single
person, and it increases the risk of adverse drug-related events in older
adults. Little is known about the epidemiology of polypharmacy at the
population level. We aimed to measure the prevalence and incidence of
polypharmacy and to investigate the associated factors.
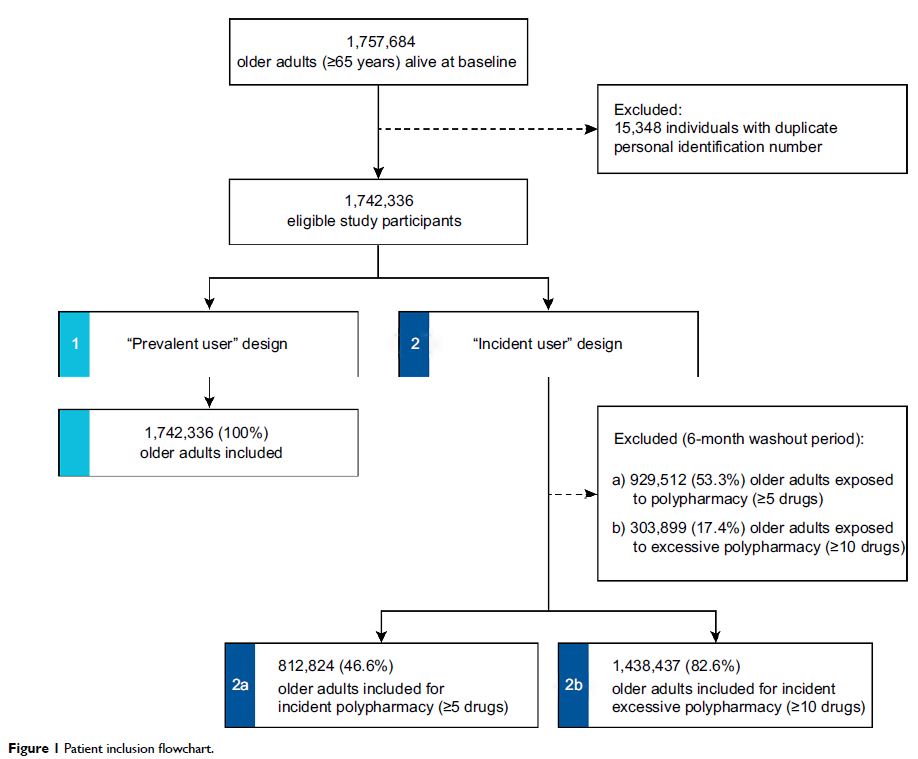
Methods: A prospective cohort study was conducted using register data with
national coverage in Sweden. A total of 1,742,336 individuals aged ≥65 years at
baseline (November 1, 2010) were included and followed until death or the end
of the study (December 20, 2013).
Results: On average, individuals were exposed to 4.6 (SD =4.0) drugs at
baseline. The prevalence of polypharmacy (5+ drugs) was 44.0%, and the
prevalence of excessive polypharmacy (10+ drugs) was 11.7%. The incidence rate
of polypharmacy among individuals without polypharmacy at baseline was 19.9 per
100 person-years, ranging from 16.8% in individuals aged 65–74 years to 33.2%
in those aged ≥95 years (adjusted hazard ratio [HR] =1.49, 95% confidence
interval [CI] 1.42–1.56). The incidence rate of excessive polypharmacy was 8.0
per 100 person-years. Older adults using multi-dose dispensing were at
significantly higher risk of developing incident polypharmacy compared with
those receiving ordinary prescriptions (HR =1.51, 95% CI 1.47–1.55). When
adjusting for confounders, living in nursing home was found to be associated
with lower risks of incident polypharmacy and incident excessive polypharmacy
(HR =0.79 and HR =0.86, p <0.001,
respectively).
Conclusion: The prevalence and incidence of polypharmacy are high among older adults
in Sweden. Interventions aimed at reducing the prevalence of polypharmacy
should also target potential incident polypharmacy users as they are the ones
who fuel future polypharmacy.
Keywords: drugs, older adults, polypharmacy, prescribing, medication,
elderly